Fatal Outcome Consequent to an Endoscopic Full Thickness Resection of a Colonic Lateral Spreading Tumor: A Case Report
AUTORI
Giovanni Oliviero, Mario Gagliardi, Marco Napoli, Orazio Labianca, Antonio D’Antonio, Mariano Sica, Attilio Maurano, Claudio Zilli
ABSTRACT
Endoscopic full-thickness resection represents an innovative procedure, used in selected patients that allows
lesions en-bloc resection with an integral wall specimen available for histopathological definition. Bleeding and
perforation are known to be the most frequent procedure-related adverse events. We report a case of enterocolonic
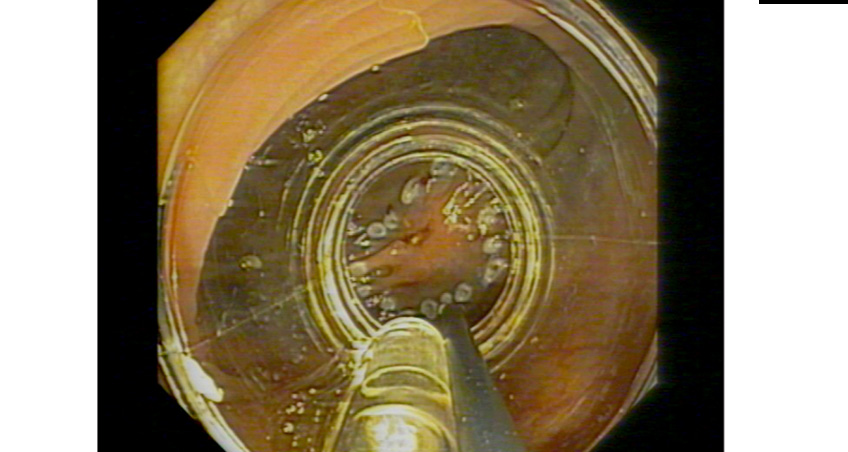
fistula as complication of an endoscopic full-thickness resection. A 77-year-old male, with a personal history of right-hemicolectomy for a colonic adenocarcinoma presented to our department for a routine colonoscopy that showed the presence of a 25 mm lateral spreading tumor localized at about 50 cm from the anal margin. A full-thickness resection of the lateral spreading tumor using the over-the-scope clip device was performed. After 4 weeks, because of abdominal pain, weight loss, diarrhea, and signs of malnutrition, the patient underwent a new colonoscopy showing hyperemic mucosa with ulcerations in all colonic segments and, at the site of the previous endoscopic full-thickness resection, an orifice of an entero-colonic fistula. The histological definition was suggestive for ulcerative proctocolitis and confirmed the presence of small bowel mucosa at fistula orifice. An intussusception at the level of fistula with consequent intestinal obstruction caused a worsening of clinical conditions and finally the patient death for a septic peritonitis. Full thickness resection represents an innovative tool for en-bloc resection of gastrointestinal tumoral lesion, but procedural complications and limitations must be considered before performing this procedure.
Oliviero G, Gagliardi M, Napoli M et al. Fatal Outcome Consequent to an Endoscopic Full Thickness Resection of a Colonic Lateral Spreading Tumor: A Case Report. Am J Case Rep. 2020;21:e922855.
SCARICA QUESTO ARTICOLO IN PDF